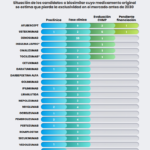
The article titled 'Spain could save millions with greater adoption of bevacizumab biosimilars' highlights that the introduction of biosimilars into the Spanish National Health System (SNHS) could generate significant savings in the pharmacological budget. According to a study published in the European Journal of Hospital Pharmacy, the implementation of bevacizumab biosimilars in the systemic treatment of cancer patients in the SNHS would lead to budget savings from the first year.
Cancer is the second leading cause of death in Europe and has a major impact on public health. Bevacizumab is an angiogenesis inhibitor approved to treat cancerous tumors and has expanded the range of biological cancer treatments. It is estimated that approximately 30% of the pharmaceutical budget in Europe is allocated to the acquisition of biological medicines. The expiration of patents on original biologic drugs has given rise to biosimilar drug alternatives.
The study used a three-year budget impact analysis model to estimate the costs of introducing bevacizumab biosimilars into the SNHS for the adult population eligible to receive such treatment. The values for population estimation were obtained from the literature and validated by a panel of experts. Only pharmaceutical costs acquired through official databases were considered in the analysis, and a sensitivity analysis was performed to evaluate the robustness of the model.
The results showed that the introduction of bevacizumab biosimilars would generate significant budget savings in the three years evaluated. In the first year, savings of €11,558,268 ($12,394,104) were estimated with a biosimilar penetration rate of 30%. In the second year, with a 50% quota, the savings would amount to €29,126,373 ($31,232,647), and in the third year, with an 80% quota, it would reach €52,361,778 ($56,148,320).
Overall, a decrease in costs for all cancers treated with bevacizumab per patient was observed after the introduction of biosimilars. Indications requiring higher doses experienced a greater impact due to the lower price of bevacizumab biosimilars. However, for indications where a greater number of patients could benefit from the use of biosimilars, such as metastatic colorectal cancer, significant cost differences were observed.
The researchers conclude that the inclusion of bevacizumab biosimilars in the Spanish health system will lead to a decrease in budget allocations for the acquisition of biological medicines, which will be notable from the first year. The savings are due to the price difference between the original bevacizumab and its biosimilars, as well as market access policies and physicians' confidence in its implementation in hospital settings.
In summary, the adoption of bevacizumab biosimilars in Spain could have a significant impact on reducing costs in cancer treatment and benefit both the health system and patients.